Breast tenderness, bloating, weight gain, emotionally crazy, on edge, a raging b*tch or just not feeling right are some of the common complaints associated with the birth control pill, which is the number one most-prescribed medication used for contraception. Birth control is simply a way of life, and the easiest and most cost effective method has always been “the pill.” But times are changing: The IUD has been around a long time, but for many, it’s the “new kid” on the block since women of all ages are now considered eligible to use it.
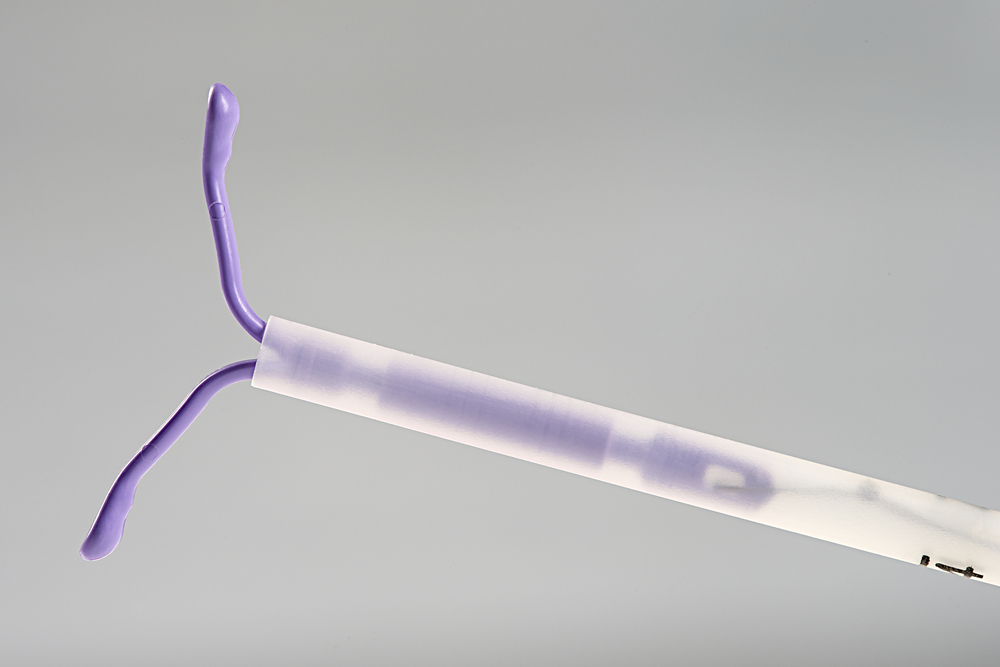
The intrauterine device (IUD) is an effective, safe, and long-term contraception. IUDs are small, flexible, and plastic, which fits nicely inside the uterus. Almost all women including teenagers now make great candidates for the IUD.
European countries have as many as 20% of women using IUDs, while Americans have only 3% of women using IUDs, even though it has just a 1% failure rate as contraception compared to the 9% failure rate of the birth control pill. Modern-day IUDs have an excellent safety record and are now commonly recommended to women.
Currently there are 3 IUDs available to women:
The copper IUD (Paraguard): This non-hormonal IUD can be used up to 10 years. You will still have monthly periods and the menstrual flow may be heavier than usual. This is perfect for those sensitive to or cannot take any kind of hormones, especially breast cancer patients.
The levonorgestrel-releasing IUD (Mirena): This progesterone releasing IUD can be used for five years. Your periods will be much lighter or non-existent as a result of the progesterone effect on the uterine lining. It is especially useful for women who have heavy or irregular menstrual cycles.
The “mini” levonorgestrel-releasing IUD (Skylar): This newest member of the IUD family can be used for three years. Similar in design to the Mirena, Skylar is smaller in size and recommended for those women who have never been pregnant. It is ideal and well-tolerated by teenagers.
How do IUDs work?
The copper IUD prevents pregnancy by stopping the sperm from going through the cervix and into the uterus and creating a sterile inflammatory reaction inside the uterine cavity. The IUDs with progesterone makes the cervical mucus thicker so sperm cannot get inside to uterus to fertilize the egg.
Here are some common myths associated with the IUD:
Myth #1: The IUD is not recommended for teens or women who have never been pregnant before.
In a recent Committee Opinion on Adolescents and Long Acting Reversible Contraception (LARC’s), the American College of Obstetricians and Gynecologists (ACOG) recommends the IUD as a “first-line” option for all women of reproductive age.
The Skylar IUD, which is smaller in size, may work best for those with a smaller uterine cavity like teens and women who have never been pregnant. We now know that IUD’s are completely safe for all women regardless of whether they have been pregnant or not.
Myth #2: Perforation of the IUD is common.
Perforation or misplacement of an IUD occurs in 1 out of every 1,000 insertions. When an IUD is not placed directly into the uterine cavity excessive cramping and pain may occur. It is best if you can have a pelvic ultrasound done following the insertion to make sure it is in its proper place.
Myth #3: The IUD can cause infertility.
The current IUDs, Paraguard, Mirena and Skylar, have been well-studied and are completely safe. Your biggest risk factor for infertility is a previous infection with Chlamydia and Gonorrhea unrelated to an IUD. IUDs do not increase your risk of getting sexually transmitted infections (STI). Prior to having an IUD inserted, it is recommended to get STI testing.
Myth #4: The IUD will make my periods heavier and more painful.
It is true that the hormone-free copper IUD, Paraguard, may make you have heavier bleeding and more cramping. The progesterone containing IUDs, Mirena and Skylar, were designed to give you a lighter or non-existent period. The Mirena IUD often gives you no period, which is a welcomed side effect for many women. In fact, the Mirena IUD is also used to treat women with irregular and heavy periods.
Myth #5: IUD insertion is difficult.
This is very individualized and depends on your pain tolerance and IUD preparation. The best time to insert an IUD is immediately following your last menstrual period. I suggest taking 600 to 800mg of ibuprofen 30 minutes prior to insertion. Once the IUD has been inserted it is best to periodically check the string at the entrance of the cervix. Just don’t pull on it!
It is always best to discuss the risks and benefits associated with IUDs as a form of contraception. Studies show that the IUD has the “highest patient satisfaction” amongst contraception users. I would say the IUD is making a serious and purposeful comeback.
Cover image courtesy of Shutterstock.




comments